May 24, 2018
Use Big Data to Improve the Healthcare Revenue Cycle

Every day, the world creates 2.5 quintillion bytes of data, according to IBM. Healthcare information accounts for a sizable portion of this data, and numbers will continue to rise. Exploding amounts of medical data, from genomic testing and large imaging studies to billions of payment transactions, are ripe for advanced systems analysis.
Bill Gates once said, “A breakthrough in machine learning would be worth ten Microsofts.” Healthcare revenue cycle management (RCM) stands to benefit immediately from big data analytics and artificial intelligence advances.
Revenue Cycle Ecosystem Challenges
Health systems face multiple challenges due to the vast amounts of data contained in electronic medical records and billing systems. Common RCM data issues include: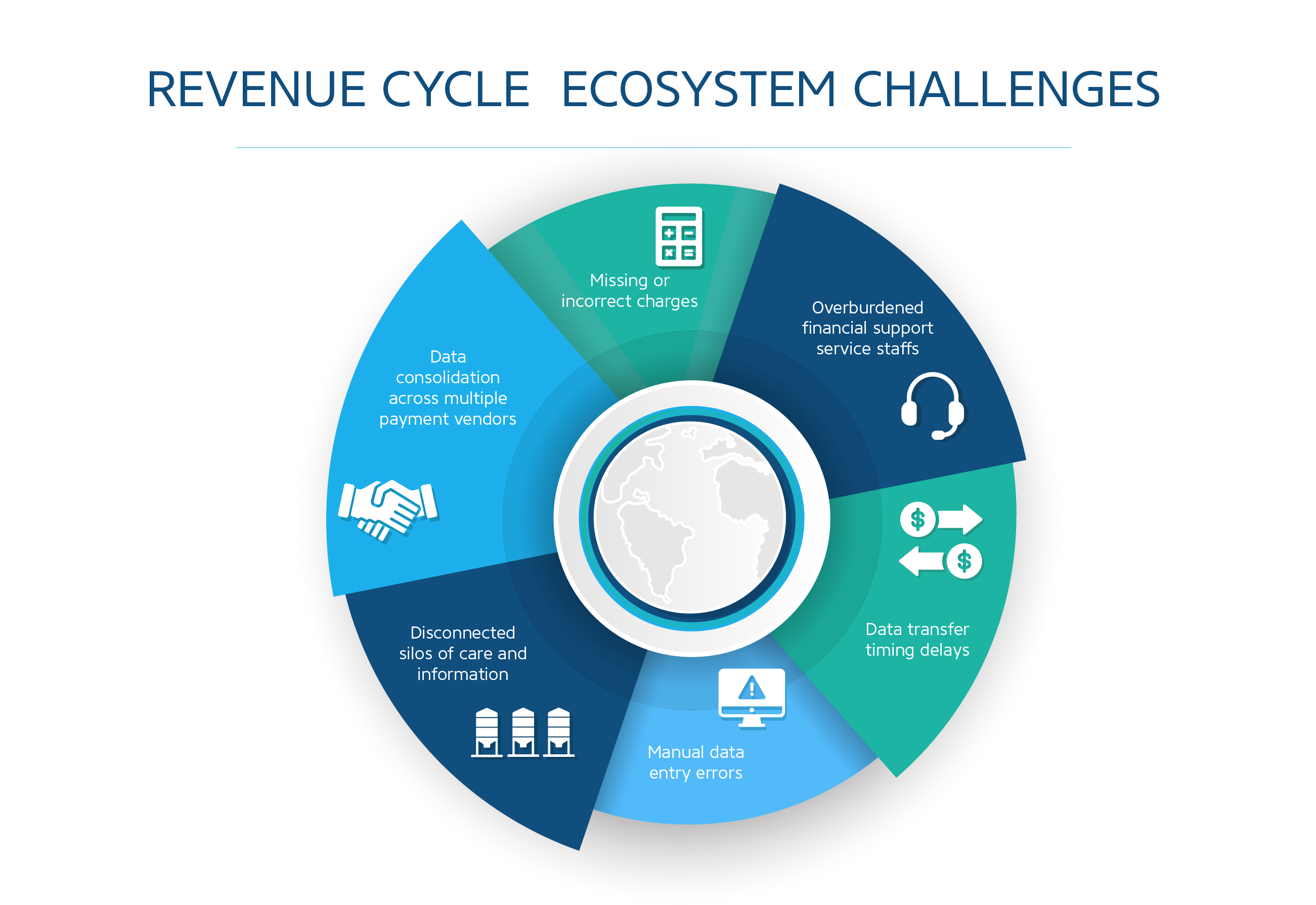
- Missing or incorrect charges. Charge capture problems can cost up to 1 percent of annual net revenue
- Data consolidation across multiple payment vendors
- Overburdened financial support service staffs
- Manual data entry errors
- Disconnected silos of care and information
- Data transfer timing delays
Big Data to the RCM Rescue
By finding and analyzing patterns in vast amounts of data using machine learning, you can improve productivity in your healthcare revenue cycle. Hospitals already use AI applications and big data analysis in the areas of insurance pre-certifications, denial prediction, and ICD-10 billing code verification.
This post discusses two impactful areas for data analysis in RCM: revenue leakage and managing multiple payment vendors.
Use Big Data to Solve Revenue Leakage Challenges
Hospitals typically lose 1 to 5 percent of net revenue due to leakage. This number is expected to grow with ICD-10, ACA, and increased out-of-pocket payment volumes.
All health systems have processes to identify revenue leakage, but many are not very effective. Manual audit reviews are time-consuming and inconsistent due to data silos and available resources. Rules-based systems, such as bill scrubbers, look only for specific pre-identified errors.
Analytics-based systems are the most efficient approach to combat revenue leakage.
An analytics-based approach uses big data and machine learning to prevent revenue leakage. It can take billing data (such as diagnostics attributes, procedure attributes, billing code attributes, charge code attributes, local hospital history, and global system history) to build a database. From there, it can match present cases with past cases, and examine the variances between them.
Once an auditor provides feedback on machine-based recommendations, the system will, in turn, learn and improve. The system can also track auditors, so it can advance the hospital’s front-end processes, in addition to correcting possible errors on the back end.
Tackling Accounts Receivable Challenges When Using Multiple Vendors
Most healthcare organizations engage in a complicated receivables process involving multiple vendors. These vendors work with healthcare organizations on boutique processes ranging from payer denials to patient collections.
Managing a cornucopia of vendors is complicated because each vendor brings distinct methodologies, touch points, interfaces, and data types. How do healthcare organizations ensure that their vendors are identifying incorrect statements and charging correct rates?
Big data comes to the rescue again. Extracting data from the vendors directly (instead of simply using provided vendor spreadsheets and reports) gives hospitals an advantage. It allows hospitals to sort through information about all their different vendors on their own and identify trends. Hospitals can view and compare their vendors’ performance data, such as their screening rates, cycle times, rejection reason summaries, and in-house application summaries from multiple angles.
Health systems can then give their vendors feedback, which will result in appropriate corrective actions that ultimately lead to higher patient satisfaction ratings. Combining data science and machine learning with frontline expertise helps complex receivables operations run faster and more profitably.
Analytics and Big Data Are in RevSpring’s DNA
We understand that, when properly harnessed, big data can motivate employees, enhance the patient financial experience, and enrich your hospital’s financial health. Our data-driven decision models streamline revenue cycle processes and financial operations to improve patient communications and profits. If you’d like to learn more about our comprehensive patient engagement and billing solutions, we’d love to help you. Request a demo to see how we can help your organization meet its goals.